18 results
The role of cognitive reserve and clinical symptoms in the association between genetic liability for educational attainment and functioning in first-episode psychosis: a mediation analysis
- Derek Clougher, Àlex G Segura, Maria Florencia Forte, Gisela Mezquida, Manuel J Cuesta, Eduard Vieta, Silvia Amoretti, Antonio Lobo, Ana González-Pinto, Covadonga M. Díaz-Caneja, Alexandra Roldán, Giovanna Fico, Elena de la Serna, Daniel Bergé, Patricia Gassó, Natalia Rodriguez, Norma Verdolini, Alfonso Tortorella, Giulia Menculini, Marta Ribasés, Miguel Bernardo, Sergi Mas, PEPs Group
-
- Journal:
- European Psychiatry / Accepted manuscript
- Published online by Cambridge University Press:
- 05 January 2024, pp. 1-31
-
- Article
-
- You have access Access
- Open access
- Export citation
Meta-analysis of the variability in the individual response to pharmacological treatments for mania in bipolar disorder
- G. Anmella, M. De Prisco, V. Oliva, M. Sanabra, L. Fortea, M. Ortuño, G. Fico, A. Murru, E. Vieta, D. Hidalgo-Mazzei, A. Solanes, J. Radua
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S84
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many studies have investigated whether there exist predictors of good response to antimanic drugs in bipolar disorder (BD). However, these factors predict response or only indicate benign illness course.
ObjectivesTo shed some light on the topic, we tested whether the response to antimanic drugs showed any variability beyond that expected by the effects of illness course and placebo.
MethodsWe included all double-blind, placebo-controlled RCTs of oral pharmacotherapies targeting adult patients with acute bipolar mania from 1991 to 2020. The primary outcome was the variance of the improvement in manic symptoms in treated individuals compared to placebo. The effect size was the log variability ratio (logVR). We performed a random-effects meta-analysis, including assessments of heterogeneity, sensitivity/cumulative/subgroup analyses, and meta-regression.
Results42 RCTs (46 comparisons) from a total of 8,438 BD patients with acute mania (53.7% male, mean age=39.3; 5,563 treatment/2,875 control groups) were included in the analysis. Individuals in active treatment groups did not show variability in the response beyond that observed in individuals under placebo (VR=1; 95% C.I.=0.97,1.03; p-value=0.97). No heterogeneity was detected between the studies (I2=0%; tau2=0%; Q=29.21; df=45; p-value=0.97). Results were similar in the leave-one-out/cumulative/subgroup analyses. Meta-regression did not show influences by age, sample size, sex, severity of manic symptoms at baseline, or clinical features (rapid cycling, mixed or psychotic features).
ConclusionsThis meta-analysis shows no evidence of differences in the individual response to treatments. These findings suggest that the average treatment effect is a reasonable assumption for the individual BD patient with acute mania. The presented article adds evidence to the equivalent results in schizophrenia-spectrum disorders, clinical high-risk state for psychosis, and major depressive disorder, not supporting classification in responders vs. non-responders. However, these findings should be balanced with results from other fields supporting such classification.
Disclosure of InterestNone Declared
Is emotion dysregulation correlated to depressive and manic symptoms of bipolar disorder? Results from a systematic review and network meta-analysis
- V. Oliva, M. De Prisco, G. Fico, A. Murru, M. Fornaro, A. Serretti, J. Radua, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S275-S276
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion dysregulation (ED) is a multidimensional construct involving the lack of awareness, understanding and acceptance of emotions, a reduced access to adaptive and appropriate strategies to modulate the intensity or duration of emotional responses, and the inability to control behaviors in accordance with desired goals when experiencing negative emotions. ED is outlined in the general population and several psychiatric disorders, including bipolar disorder (BD), and influences its clinical course and management, quality of life, and daily social functioning.
ObjectivesThe objective of this systematic review was to examine the correlations between maladaptive (i.e., positive and negative rumination, negative focus, risk taking behaviors, suppression, and dampening) and adaptive (i.e., cognitive reframing, adaptive coping, and acceptance) strategies of emotion regulation (ER) and depressive and manic symptoms of BD.
MethodsWe searched the literature from inception to April 12, 2022, and included studies focusing on ER/ED assessed with a validated scale. We conducted multiple pairwise meta-analyses for correlations between ED dimension (or overall ED) and the measures of depressive and manic symptoms of BD, and separate Bayesian network meta-analyses to examine which aspects of emotion regulation were most closely associated with depressive and manic symptoms of BD. The Pearson’s r coefficients were adjusted using sample-size weights and Fisher’s r-to-z transformed was conducted.
ResultsA total of 13,826 records was identified and, after duplicate removal and title/abstract evaluation, 442 were explored at the full text. Sixteen studies were finally included. Results from pairwise meta-analyses are shown in Figure 1, results from network meta-analyses in Figure 2 and 3. Both depressive and manic BD symptomatology were found to be related to maladaptive ER strategies, with the only difference of positive rumination, associated only to manic symptoms. Negative rumination and risk-taking behaviors were the strategies more correlated to both manic and depressive symptoms, as confirmed by both pairwise metanalyses and network metanalyses. On the other hand, depressive symptomatology appeared more correlated with decreased adaptive strategies than manic symptomatology.
Image:
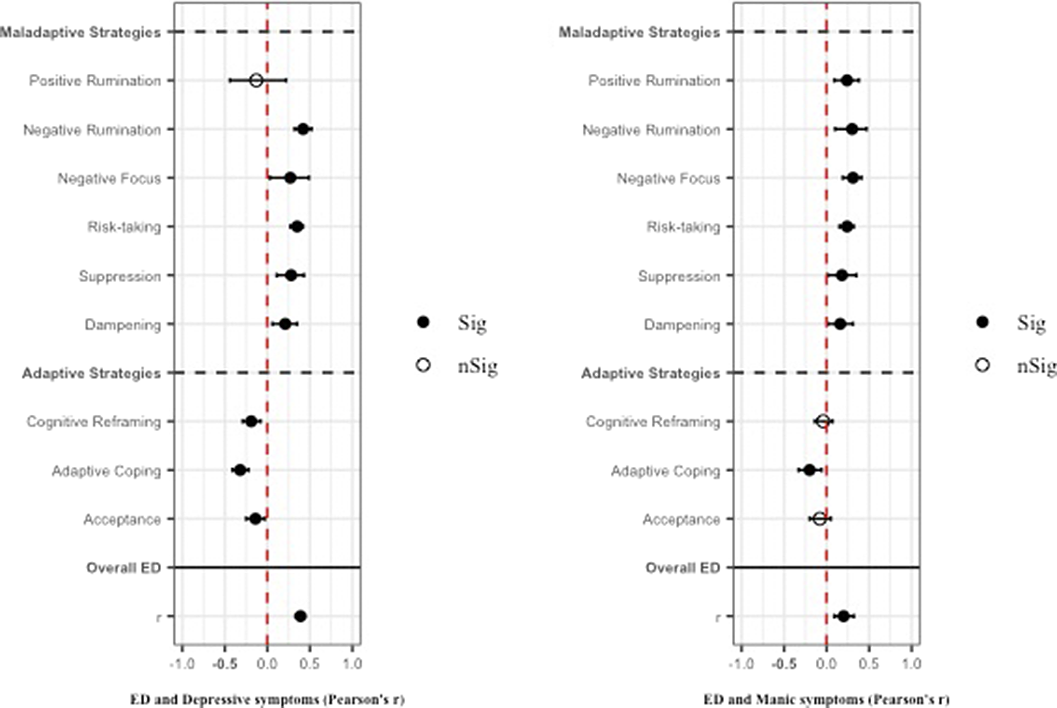
Image 2:
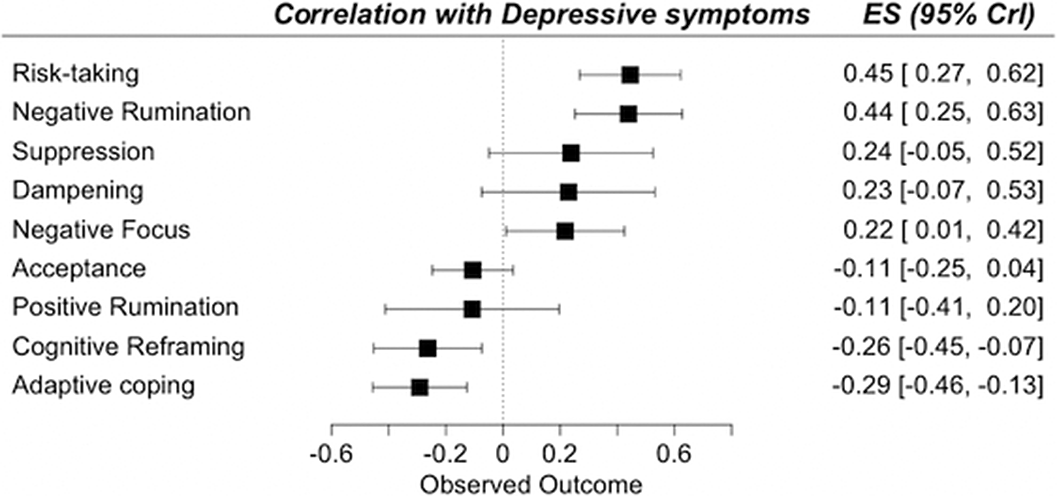
Image 3:
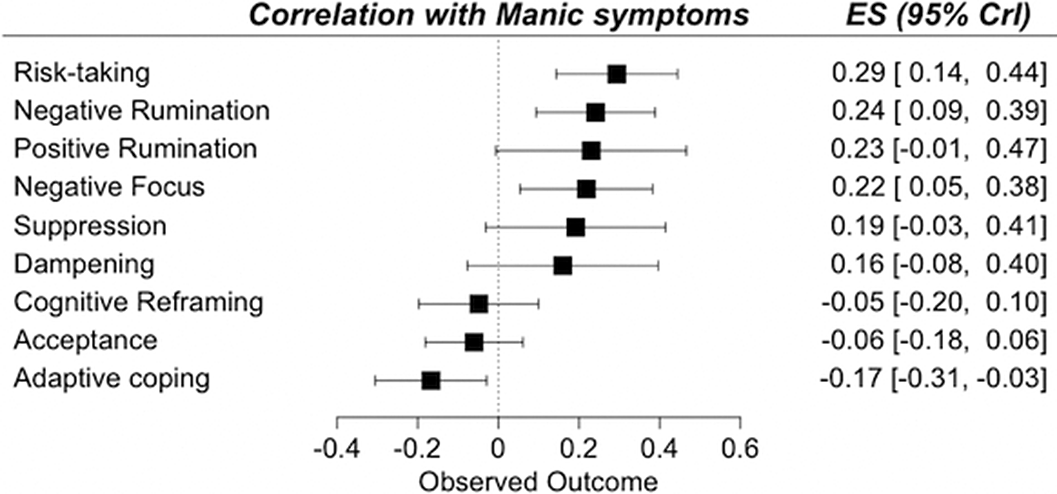 Conclusions
ConclusionsED has a significant correlation with BD symptomatology, therefore it should be explicitly considered during clinical assessment, diagnosis, and intervention on BD, and specific treatments should be implemented. More studies, and with longitudinal design, are needed to better explore these associations and their causal direction. In addition, future studies should mainly focus on the complex interactions between cognitive, social, and cultural aspects, and biological correlates to improve knowledge on a topic that is still poorly investigated.
Disclosure of InterestV. Oliva: None Declared, M. De Prisco: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda, M. Fornaro: None Declared, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris
Does bipolar disorder differ from other mental illnesses in terms of emotion dysregulation? A systematic review and meta-analysis
- M. De Prisco, V. Oliva, G. Fico, J. Radua, I. Grande, N. Roberto, G. Anmella, D. Hidalgo-Mazzei, M. Fornaro, A. de Bartolomeis, A. Serretti, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S571-S572
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion regulation (ER) is the ability to assess, monitor, or modify emotional reactions to achieve a goal (Gross. Psychological inquiry 2015; 26 1-26). When ER strategies are rigidly or maladaptively applied, emotional dysregulation (ED) can occur (Thompson. Development and psychopathology 2019; 31 805-815). ED is common in people diagnosed with bipolar disorder (BD), but it can also be described in other clinical populations given its transdiagnostic nature. Numerous aspects of ED have been described in BD (De Prisco et al. Neuroscience & Biobehavioral Reviews 2022; 104914), but it is unclear whether these manifest similarly in other conditions such as major depressive disorder (MDD) or borderline personality disorder (BPD), or whether they are specific to BD.
ObjectivesThe objective of this systematic review and meta-analysis is to examine the literature comparing BD with other psychiatric disorders in terms of ED, focusing on those studies using validated clinical tools.
MethodsA systematic search from inception to April 28th, 2022, was conducted exploring the PubMed/MEDLINE,EMBASE, Scopus, and PsycINFO databases. Those studies providing quantitative data on ED in people diagnosed with BD and compared with clinical groups were eligible for inclusion. No restriction about age, sample size, or language were applied. Random effect meta-analyses were conducted, and effect sizes were calculated as standardized mean differences (SMD).
ResultsA total of 3,239 records was identified and, after duplicate removal and title/abstract evaluation, 112 were explored at the full text. Twenty-nine studies were finally included, and it was possible to perform a meta-analysis with twenty-two (145 comparisons) of them. Only studies comparing BD with MDD, and BPD provided sufficient data to perform a meta-analysis. People with BD did not differ from people with MDD in most of the comparisons considered. However, BD patients presented higher positive rumination (two comparisons: SMD=0.46; CI=0.27, 0.64; p=8.5e-07; I2=0%; and SMD=0.34; CI=0.15, 0.52; p=2.7e-04; I2=0%) and risk-taking behaviors (SMD=0.48; CI=0.27, 0.69; p=8.11e-06; I2=0%). In contrast, people with BPD displayed an overall higher degree of ED (SMD=-1.22; CI=-1.94, -0.5; p=9.1e-04; I2= 90.7) and used fewer adaptive ER strategies. Additionally, higher levels of self-blaming (SMD=-0.80; CI=-1.11, -0.50; p=2.68e-07; I2=0) and impulsive behavior (SMD=-0.76; CI=-0.89, -0.63; p=5.4e-29; I2=0) were observed.
Image:
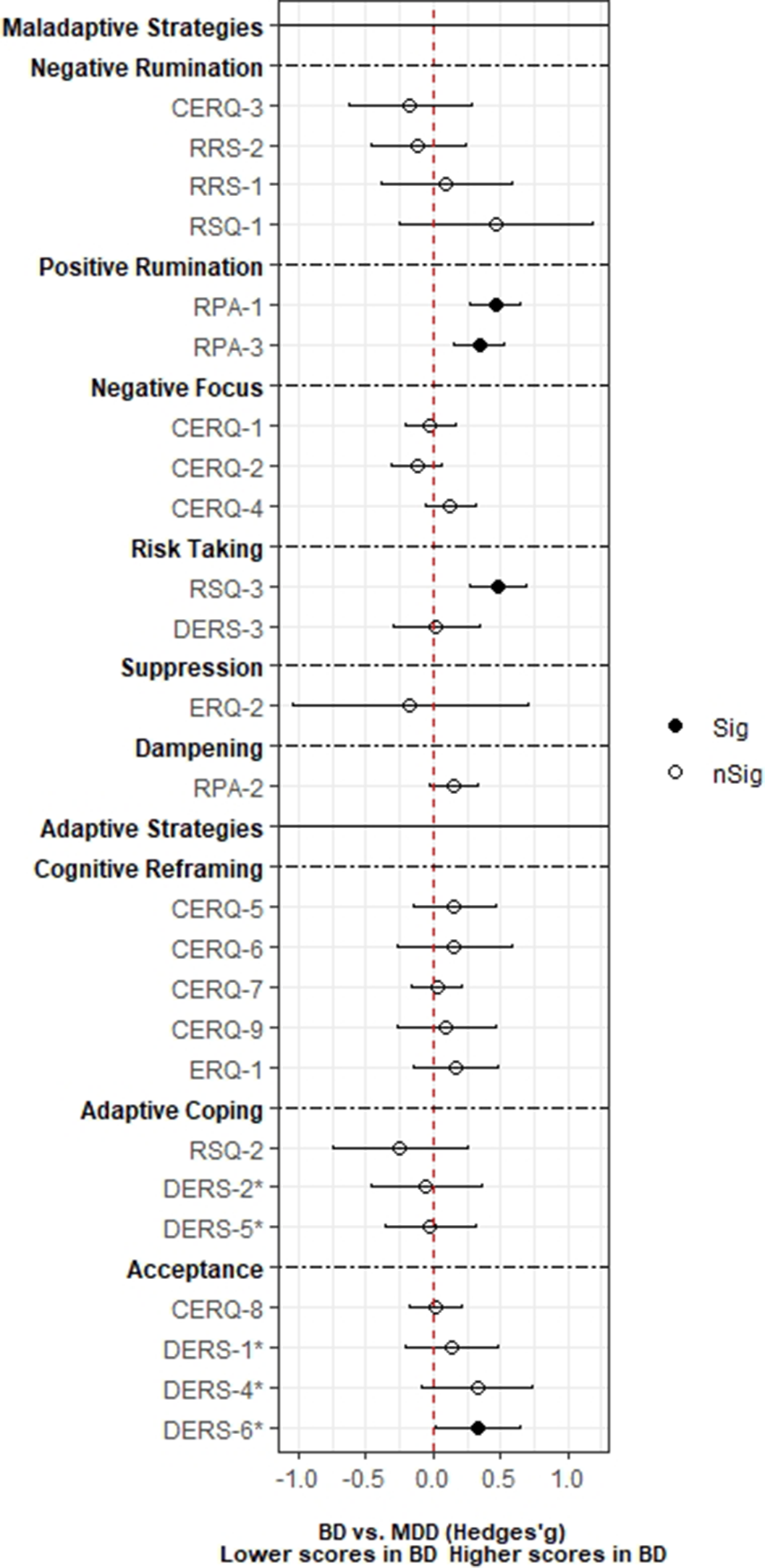
Image 2:
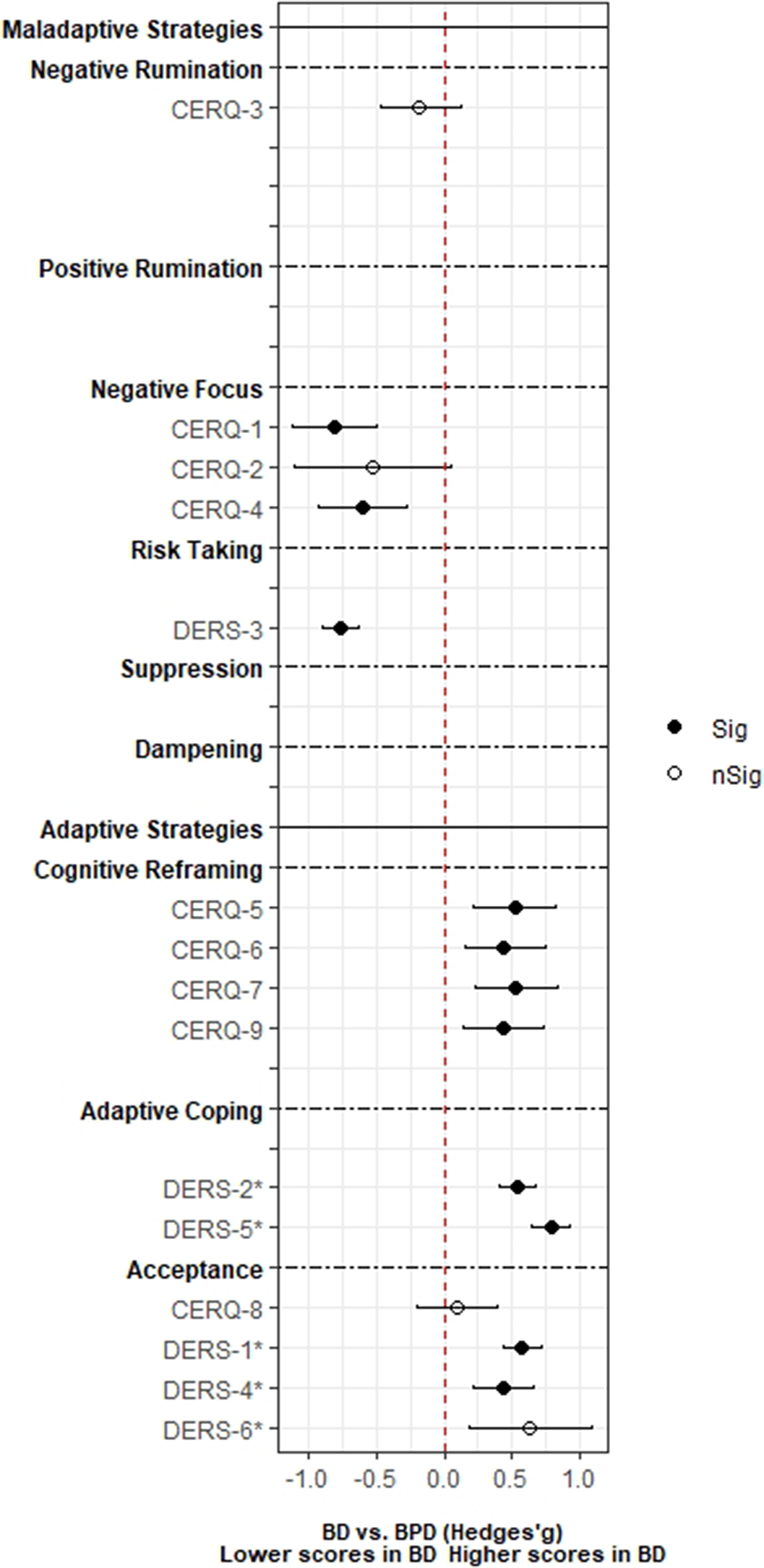 Conclusions
ConclusionsED is a trans-diagnostic construct that spans a continuum of different psychiatric disorders. Outlining the specific clinical features of one disorder versus another may help future research to increase our knowledge of these issues and develop new treatment strategies to reduce the clinical burden of these patients.
Disclosure of InterestM. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdirección General de Evaluación y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR ); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Consultant of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare, N. Roberto: None Declared, G. Anmella Grant / Research support from: Rio Hortega 2021 grant (CM21/00017) from the Spanish Ministry of Health financed by the Instituto de Salud Carlos III (ISCIII) and co-financed by the Fondo Social Europeo Plus (FSE+), Consultant of: Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, D. Hidalgo-Mazzei Grant / Research support from: Juan Rodés JR18/00021 granted by the Instituto de Salud Carlos III (ISCIII), M. Fornaro: None Declared, A. de Bartolomeis Consultant of: Janssen, Lundbeck, and Otsuka and lecture fees for educational meeting from Chiesi, Lundbeck, Roche, Sunovion, Vitria, Recordati, Angelini and Takeda; he has served on advisory boards for Eli Lilly, Jansen, Lundbeck, Otsuka, Roche, and Takeda, Chiesi, Recordati, Angelini, Vitria, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda
Consultation trends in patients admitted to a Psychiatric Emergency Service before and during COVID-19 pandemic
- M. Gomez Ramiro, A. Gimenez, G. Fico, M. Sague Vilavella, M. Valenti, M. Vazquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S591-S592
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The COVID-19 outbreak had significant implications worldwide, including mental health. Consultations in the Emergency Service of the Hospital Clínic of Barcelona varied in terms of reasons for consultations, psychopathology, and other aspects, before and during the pandemic.
ObjectivesThis study aims to assess differences in the profile of patients admitted within the last three years to the Psychiatric Emergency Service of a third-level hospital, in order to analyze variations in the number of patients visited, diagnoses and admissions throughout the different seasons.
MethodsAll adults admitted from 2019 to 2021 to the Psychiatric Emergency Service of Hospital Clínic of Barcelona, Spain, were retrospectively included for analysis and divided into three groups depending on the year they attended the Emergency Service. SPSS v25.0 and R statistics were used in order to compare differences between groups.
ResultsA total of 13677 adult individuals who attended the psychiatric emergency service of Hospital Clínic of Barcelona between 2019 and 2021 were included in the analysis. 4814 patients were visited in 2019, 4007 in 2020 and 4856 in 2021. The majority of patients were male (50.1%), with a mean age of 40.47 years (SD 15.83). In terms of acute admission rates, 24.6% of the total sample were hospitalized in an acute psychiatric unit, whereas in the spring of 2020, 34.3% of patients attending the Emergency Service were hospitalized. This revealed significant differences when compared with spring of 2019 and 2021 and with the rest of seasons (p<0.05). With regard to suicide attempts and intentional poisonings, significant differences were only observed between winter of 2019, with the lowest rate, and autumn of 2020, with the highest proportion. In spring of 2019, the lowest rate of patients attending with suicidal ideation was observed, which showed significant differences compared to winter of 2020, spring of 2021, summer of 2021 and autumn of 2021 (p<0.05). Also, statistically significant differences between winter of 2019 and summer of 2021 and also between summer of 2019 and summer of 2021 were observed, with the highest rate in the last one. No significant differences were observed in rates of patients with severe mental disorders visited.
ConclusionsThe COVID-19 pandemic and the situation of lockdown lead to an overall reduction in the overall consultations to the Emergency Service, being this reduction non-significant in patients with severe mental disorders, such as psychotic disorders. In addition, our study shows a decrease in consultations with suicidal ideation in summer of 2019 and a significant increase in summer of 2021. In contrast, an increased tendency in suicide attempts was not observed.
Disclosure of InterestNone Declared
Changing trends of suicide mortality from 2011 to 2019: an analysis of 38 European Countries
- G. Fico, A. Gimenez-Palomo, R. Andra Bursan, C. R. Ionescu, F. Kraxner, P. Rolland, S. Gomes-Rodrigues, M. Batković, E. Metaj, S. Tanyeri Kayahan, A. Mamikonyan, P. Paribello, A. K. Sikora, C. M. Platsa, M. Spasic Stojakovic, A. H. Halt, M. Az, N. Ovelian, K. Melamud, M. Janusz, K. Hinkov, C. Gramaglia, J. Beezhold, J. L. Castroman, C. Hanon, D. Eraslan, E. Olie
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S85-S86
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a serious public health problem since it accounts for nearly 900,000 deaths each year worldwide. Globally in 2019, 10.7 persons out of 100,000 died by suicide. Psychiatric disorders are related to an overwhelming proportion of these cases. In the last years, several specific interventions and action plans for suicide prevention have been implemented in a number of European countries.
ObjectivesOur aim was to analyze recent epidemiologic trends of suicide mortality rates in Europe.
MethodsAnnual national statistics of suicide mortality rates derived from Eurostat public databases from 2011 to 2019 were analyzed for 38 European countries. The suicide mortality rate was estimated per year/100,000 population. Linear regression models were used to study temporal trends of suicidal mortality. Analyses were performed using RStudio.
ResultsAvailable data show a statistically significant reduction in suicide mortality rates from 2011 to 2019 in 15 European countries, and a significant increase for Turkey (ES=0.32, SD=0.06, p=0.037) (Fig 1). The greatest significant decrease was reported in Lithuania (ES=-1.42, SD=0.02, p=0.02), followed by Hungary (ES=-1.13, SD=0.11, p=0.0007), Latvia (ES=-0.76, SD=0.11, p=0.007), and Poland (ES=-0.73, SD=0.10, p=0.001). Italy reported the lowest significant reduction in suicide mortality rates (ES=-0.13, SD=0.018, p=0.003). The remaining 16 countries showed no significant changes in suicide mortality trends.
Image:
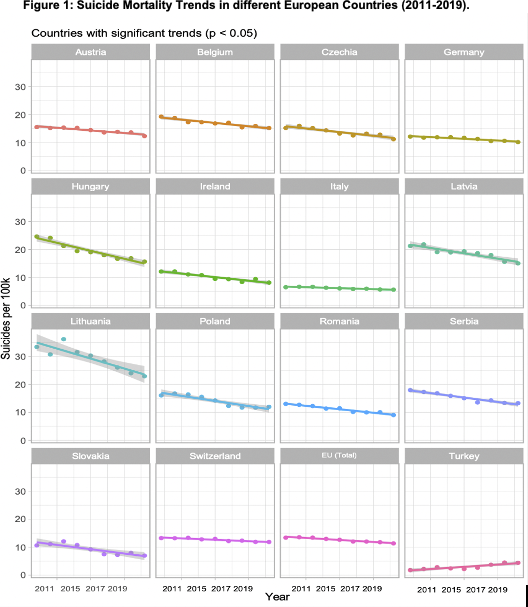 Conclusions
ConclusionsIn the last years, Europe registered an overall reduction in reported suicide rates. However, more recent data (i.e., suicide rates after COVID-19 pandemic, age and sex-related effect on suicide rates) should be analyzed and used to implement future recommendations. Current and future suicide prevention strategies aim to contribute to a greater reduction of suicide rates in the different European countries.
Disclosure of InterestNone Declared
A family history of suicide in bipolar disorders: powerful, powerless
- M. Sagué Vilavella, G. Fico, G. Anmella, A. Giménez, M. Gómez Ramiro, M. T. Pons Cabrera, S. Madero, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S387
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
When completing the medical record of a patient with bipolar disoder (BD), hardly anything is more impacting than a family history of completed suicide (FHS). In fact, FHS is a main risk factor for personal suicide attempts and death in this population. There are few modifiable protective factors against suicide in BD, such as lithium treatment and absence of substance abuse.
ObjectivesWe aimed to explore the relationship between a FHS and clinical characteristics in patients with BD. Given the impact that FHS has on the individual and on healthcare professionals, we hypothesized that it would modify behaviors towards a higher prevalence of the modifiable protective factors against suicide, namely more treatment with lithium and less drug addiction.
MethodsThis is a cross-sectional study that included all patients with BD that were followed up in a specialised unit between 1998 and 2020. Only subjects with complete information on FHS were retained for the analysis. We assessed sociodemographic and clinical data and described it with measures of frequency, central tendency and dispersion. Differences between subjects with and without FHS were calculated with χ², Fisher’s exact test and Student’s t-test as appropriate. We set the significance level at p≤0.05. All tests were two-tailed.
ResultsThe sample consisted of 480 subjects with a mean age of 45.9 years (standard deviation 14.4, range 18-88), of which 54.4% (n=261) were women. 69.2% (n=332) had a diagnosis of BD type I and 30.8% (n=148) of BD type II. 77 subjects (16%) had a FHS. Regarding differences between groups, those with relatives who had committed suicide did not show statistically significant differences in terms of sociodemographic variables (age, gender, civil status, employment) or key clinical features (type of BD, illness duration, psychotic features, predominant polarity, rapid cycling, number of lifetime manic and depressive episodes, comorbid personality disorder), neither did they have a higher use of lithium (55.8% vs 59.3%, p=0.572) nor lower substance use disorder (10.9% vs 15.5%, p=0.34). Predictably, people with FHS had a higher prevalence of family history of mental and affective disorders (96.1% vs 70.9%, p<0.001; 86.3% vs 56.3%, p<0.001) and of stressful life events (71.6% vs 58.9%, p=0.05). Personal lifetime suicide attempts also tended to be higher (36.4% vs 26.7%, p=0.088).
ConclusionsContrary to our hypothesis, in our sample of subjects with BD a FHS was not associated with a higher prevalence of the modifiable protective factors against suicide. Therefore, although suicide has a major impact both in families and healthcare professionals, our results suggest it does not modify attitudes towards prevention in a real-life scenario. The main limitation of our study is its cross-sectional design, which does not allow for causal inference. In conclusion, there is room for improvement in the fight against suicide.
Disclosure of InterestNone Declared
Lifetime number of affective episodes and functioning in a cohort of patients with bipolar disorder: A cross-sectional study
- L. Colomer, G. Fico, F. Gutiérrez, E. Pujal, N. Baldaquí, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S384
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cognitive impairment has been commonly found in patients with bipolar disorder (BD).(1) Recent evidence supports the view that global and cognitive functioning decrease as a function of number of prior mood episodes, but the relationship is still not clear. (2)
ObjectivesWe conducted a cross-sectional study to explore the associations between the lifetime number of affective episodes and functioning, in particular, cognitive functioning in a cohort of patients with BD.
MethodsAdult patients with BD were recruited if euthymic for at least 3 months. Socio-demographic and clinical variables were recollected at the baseline evaluation. Functioning was evaluated at baseline with the functioning assessment short test (FAST). The strength of the association between the lifetime number of affective episodes and FAST subscores was explored with Spearman’s correlation test. Linear regression was computed using cognitive functioning as the dependent variable and a set of clinically relevant variables including the lifetime number of affective episodes as independent variables after controlling for illness duration.
Results261 BD patients were recruited. Patients with a higher number of lifetime affective episodes showed a significant positive correlation with higher FAST global score (r=0.334, p<0.001) and FAST cognitive functioning subscore (r=0.331, p<0.001). At the linear regression, a higher number of affective episodes was associated to worse cognitive functioning (b=0.037, 95%CI [0.011-0.064], p=0.005).
ConclusionsPoor cognitive functioning in BD could be the result of multiple affective relapses. A timely diagnosis with subsequent effective prophylactic treatment may prevent poor functional outcomes in real-world patients with BD.
Disclosure of InterestNone Declared
Psychotropic drug repurposing for COVID-19: a systematic review
- U. Isayeva, G. Fico, S. Gomes-Da-Costa, M. Sagué Villavella, A. Gimenez, M. Manchia, A. Murru
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S337
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Recently, several antidepressants, mood stabilizers, and antipsychotics have been suggested to have favorable effects in the treatment of COVID-19.
ObjectivesThe aim of this systematic review was to collect evidence from preclinical and clinical studies concerning the scientific evidence for the repurposing of psychotropic drugs in COVID-19 treatment.
MethodsTwo independent authors searched PubMed-MEDLINE, Scopus, PsycInfo, Clinical Trial Registration Site US (ClinicalTrials.gov) databases, and reviewed the reference lists of articles for eligible articles published up to May 31st, 2021. All preclinical and clinical studies on the effect of any psychotropic drug on Sars-CoV-2 or patients with COVID-19 were included. The Newcastle-Ottawa scale was used for the quality assessment of clinical studies. This systematic review adheres to the PRISMA guidelines.
Results22 studies were included in the synthesis: 9 clinical studies, 9 preclinical studies, and 4 computational studies. The use of antidepressants, both SSRI and non-SSRI, was associated with a reduced risk of severe complications of COVID-19. Several antipsychotics showed an increased risk for both Sars-CoV-2 infection and severe complications during COVID-19.
ConclusionsThe current evidence supports a potential anti-SARS-CoV-2 role for several antidepressants, while the evidence on mood stabilizers or antipsychotics remains controversial. Drug repurposing proved highly successful in response to the current pandemic and psychotropic medications are widely used in clinical practice with well-known safety and tolerability profiles, showing antiviral, immunomodulatory, and anti-inflammatory properties, being perfect candidates for possible treatment of COVID-19. Further research will deliver optimized and specific therapeutic tools that will increase the preparedness of health systems for possible future epidemics.
DisclosureNo significant relationships.
Emergency Psychiatry before and during COVID-19 pandemia
- A. Giménez-Palomo, M. Sagué, G. Fico, M. Gómez-Ramiro, M. Vázquez
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S277
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The COVID-19 pandemic had a significant impact worldwide. Consultations in the Emergency Service of the Hospital Clínic of Barcelona varied in terms of reasons for consultations, psychopathology, and other aspects, before and after the pandemic.
ObjectivesTo examine changes in the profile of patients admitted before and during the COVID-19 pandemic to our Psychiatric Emergency Service.
MethodsAll children, adolescent and adult psychiatric inpatients admitted from December 4th 2019 to March 31st 2021 to the Psychiatric Emergency Service of Hospital Clínic of Barcelona, Spain, were retrospectively included for analysis and divided into two groups –groups 1 or 2- including the first one all patients who attended before lockdown and the second group those who attended during the pandemic.
ResultsA total of 1991 patients were included -1224 in the first group and 767 in the second group. The majority of patients were male (52.08%), with a mean age of 41.21 years (SD 16.53). A proportion significantly higher of men was found in the second group (p<0.05). The proportion of patients consulting with substance use disorders was significantly higher in the second group (p<0.05). Patients from the second group presented a significantly higher proportion of admissions in an acute psychiatric ward (p<0.05), and also a significantly higher proportion of consultations of patients with dementia (p<0.05).
ConclusionsThe COVID-19 pandemic lead to a significant reduction in the overall consultations, with a higher proportion of severe cases. The lack of availability of caregivers and telework might have influenced the increase in consultations of patients with dementia.
DisclosureAG has received travel and financial support from Janssen, Otsuka-Lundbeck and Angelini, and research support from Instituto de Salud Carlos III, and declares no support related with the subject of this presentation.
Bipolar disorders and suicide: stumbling twice with the same stone?
- M. Sagué-Vilavella, G. Fico, G. Anmella, A. Giménez-Palomo, M. Gómez-Ramiro, M. Pons Cabrera, S. Madero, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S222-S223
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is the most terrible outcome of bipolar disorders (BD). It impacts families and healthcare professionals deeply. Family history of suicide (FHS) is one of its main risk factors, whereas lithium treatment and absence of substance use disorders (SUD) are two of its few modifiable protective factors.
ObjectivesTo explore the relationship between FHS and clinical characteristics in BD. We hypothesized that FHS would be associated with less SUD, higher rates of lithium treatment and shorter duration of untreated illness (DUI).
MethodsCross-sectional analysis of subjects with BD followed-up in a specialised outpatient unit (Barcelona, October’08-March’18). We described data with measures of frequency, central tendency and dispersion, and we used χ², Fisher’s test and t-tests for comparisons.
ResultsThe sample consisted of 83 subjects, 56.6% males, mean age 41.9 years (SD 12.7). 74.7% (n=62) had a diagnosis of BD-I and 25.3% (n=21) of BD-II. 11 subjects (13.3%) had FHS. Those with FHS did not show significant differences in sociodemographic data, DUI (58.5+/-60.4 vs 38.19+/-84.9 months, p=0.341), lithium use (72.7% vs 73.6%, p=0.95) or SUD (27.3% vs 23.6%, p=0.79). There were differences in terms of lifetime suicide attempts (54.5% vs 20.8%, p=0.026), family history of mental disorders (100% vs 69.4%, n=0.032).
ConclusionsContrary to our hypothesis, FHS was not associated with the modifiable protective factors against suicide (namely, less SUD and more lithium prescription). Similarly, we did not find an association with earlier access to mental health services at symptom onset (DUP as proxy). Therefore, our results suggest FHS does not modify attitudes towards prevention.
DisclosureNo significant relationships.
EPA-1116 - Obesity Affects Cognitive Performances Even in the Absence of Obvious Psychopathological Alterations. A Comparison with Schizophrenia Subjects and Non-Affected Controls
- R. Balletta, C. Cucciniello, M. Formato, G. Pecoraro, S. Orlando, G. Mazzola, C. Avagliano, G. Fico, A. De Bartolomeis, F. Micanti, F. Iasevoli
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Obesity has been associated with cognitive impairment. However, it is not clear whether cognitive impairment may depend on concomitant psychopathology, since several psychiatric conditions, e.g. schizophrenia, include cognitive deficits among their manifestations.
Objectives:To assess cognitive performances and psychopathology in obese patients, and to compare cognitive alterations in obese patients with those in schizophrenics and controls.
Aims:To compare cognitive performances in obese patients to normal percentiles. To provide an analysis of correlation with specific psychopathological domains. To evaluate whether cognitive performances in very obese patients were different from those in schizophrenia patients and non-affected controls.
Methods:88 obese patients were included. Exclusion criteria were: axis I and II diagnosis; severe medical, neurological, or endocrinology conditions. Patients underwent an extensive battery of cognitive tests and completed the Toronto Alexithymia Scale (TAS-20), the Barratt Impulsiveness Scale (BIS-11), the Beck Depression Inventory (BDI), the State-Trait Anxiety Inventory (STAI). In the second part of the study, very obese patients (BMI>40; n=16) were compared for cognitive performances to schizophrenia patients (n=16) and non-affected controls (n=17).
Results:Obese patients performed at low percentiles (<15) on the Problem Solving and the Social Cognition tasks. Mean scores on psychopathology rating scales did not reach abnormal values. No correlation was found with psychopathology. When compared to schizophrenics, no significant differences were found in performances on spatial working memory.
Discussion:Obese patients show cognitive alterations even in the absence of abnormal psychopathology. Very obese patients share cognitive alterations with schizophrenia patients, which may imply common neurobiological basis.
Worse Comes to Worst in Schizophrenia: Treatment Resistant Schizophrenia Patients Show Greater Impairment in Functional Milestones of Everyday Living Compared to Other Psychiatric Disabling Conditions
- F. Iasevoli, S. Giordano, R. Balletta, L. Avvisati, M.V. Formato, E. Prinzivalli, G. Fico, C. Avagliano, M. Caiazzo, C. Tomasetti, A. De Bartolomeis
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Schizophrenia patients experience severe difficulties in a range of common activities, defined 'functional milestones' (i.e. marriage, employment, self-supported living).
Objectives/AimsThis study investigated the impairment in functional milestones in treatment resistant schizophrenia (TRS), compared to other severe disabling psychiatric conditions. Moreover, we evaluated whether multiple clinical and psychopathological features may be predictors of outcome in such functional milestones.
Methods157 patients were enrolled and subdivided in four groups by diagnosis: anxious-depressive spectrum, bipolar disorder spectrum, schizophrenia responder patients, TRS patients. Demographic, clinical and social data were collected. Patients underwent psychopathological, psychosocial and cognitive functioning assessments. Positive and Negative Syndrome Scale (PANSS), Personal and Social Performance (PSP) scale, Quality of Life Enjoyment and Satisfaction Questionnaire (Q-LES-Q), List Learning task for Verbal Memory, Digit Sequencing task for Working Memory, Category Instances task for Verbal Fluency and Tower of London task for Problem Solving were administered. Data were analyzed by ×2 test, ANOVA test and Kruskal-Wallis test. Stepwise multivariate regression was used to correlate functional outcomes to clinical and psychopathological variables.
ResultsTRS patients were more severely impaired in all psychosocial areas explored, were exposed to higher antipsychotic doses, had a higher number of hospitalizations, had higher scores on psychopathological rating scales and performed worse on the verbal memory task. Outcomes in functional milestones were more correlated to clinical/psychopathological variables in TRS than in the other groups.
ConclusionsPsychosocial impairment, clinical, and psychopathological features generate a vicious circle in TRS, which is less evident in other disabling psychiatric conditions.
EPA-1118 - Knowledge of the Illness and Its Relations with Quality of Life, Social Functioning, Cognitive Performances, and Adherence in Psychotic Patients: Toward Effectiveness-Focused Interventions
- L. Avvisati, G. Latte, V. Gilardi, S. Giordano, R. Balletta, E. Prinzivalli, E.F. Buonaguro, C. Elce, R. Rossi, M.V. Formato, R. Acampora, C. Avagliano, G. Fico, G. Mazzola, C. Tomasetti, A. De Bartolomeis, F. Iasevoli
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Psychosocial factors are often underestimated in psychotic patients, although they may profoundly influence (and be influenced by) clinical presentation and effectiveness of therapeutic interventions in these people.
Objectives:To investigate relevance, relationship with clinical presentation and overall quality of life of multiple psychosocial factors in psychotic patients.
Aims:To evaluate whether knowledge about the illness and utilization of health services are defective in psychotic vs. non-psychotic patients and whether these correlates with the type of psychotic symptoms, cognitive performances, global social functioning, quality of life, and acceptance of pharmacotherapy.
Methods:Approximately 110 patients were enrolled after written informed consent. Patients were administered the Positive and Negative Syndrome Scale (PANSS), the Personal and Social Performance scale (PSP), the Drug Attitude Inventory (DAI), the Quality of Life Enjoyment and Satisfaction Questionnaire (Q-LES-Q). All patients were also screened for cognitive performances. Patients and relatives completed a questionnaire on knowledge about the illness and on the level of utilization of mental health services. Patients were subdivided in psychotic (cases) and non-psychotic (controls) based on their score on the PANSS.
Results:Psychotic patients and their relatives showed lower levels of knowledge about the illness. These features were associated with the other variables assessed in a very complex and multidimensional model of reciprocal influences.
Conclusions:Lack of response to pharmacological treatments and to overall therapeutic interventions in psychotic patients may also depend on multiple psychosocial factors, which may be carefully investigated and become the target of adjunctive, effectiveness-focused interventions.
Attachment and hypothalamus-pituitary-adrenal axis functioning in patients with eating disorders
- F. Monaco, A.M. Monteleone, F. Pellegrino, V. Ruzzi, G. Fico, U. Volpe, P. Monteleone
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, pp. S551-S552
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Attachment theory suggests that different attachment styles influence the development of individual's self-esteem and modulate the individual's ability to manage stressful events by responding with adequate affective adjustment. High levels of insecure attachment are present in adults with Eating Disorders (EDs).
ObjectivesThe variables that mediate the association between attachment style and EDs have not been investigated enough. The possibility exists that the endogenous stress response system is involved.
AimsTo appraise the role of the endogenous stress response system, we studied the effect of attachment styles on the hypothalamus-pituitary-adrenal (HPA) axis functioning in ED patients.
MethodsFifty- two women with EDs and 25 healthy women completed the ECR questionnaire to assess their attachment style. Saliva samples were taken in the morning to measure the Cortisol Awakening Response (CAR). Moreover, the saliva cortisol response to the Trier-Social-Stress-Test (TSST) was measured in 30 ED patients and 15 healthy controls.
ResultsPatients with avoidant attachment showed an increased CAR compared to both healthy controls and to patients with anxious and secure attachment styles. In the initial TSST phase, cortisol levels decreased in the secure attachment group but not in patients with avoidant attachment. In the TSST stress response phase, the cortisol raise was higher in insecure patients and delayed in avoidant ones.
ConclusionsIn adults with EDs, attachment styles affect the HPA axis functioning and this could have a role in the pathophysiology of EDs.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Investigation of endocannabinoids and endocannabinoid-related compounds in obese subjects during an hedonic eating experimental test
- V. Ruzzi, A.M. Monteleone, F. Monaco, G. Fico, A. Cervino, U. Volpe, P. Monteleone
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S551
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Hedonic eating refers to the consumption of food just for pleasure and not for energetic needs. Endocannabinoids and endocannabinoid-related compounds play an important role in food-related reward and are likely involved in hedonic eating.
ObjectivesIn a previous study we found that in normal weight healthy subjects plasma levels of 2 arachidonoylglycerol (2-AG) decreased progressively after food ingestion in both hedonic and non-hedonic eating condition, but they were significantly higher in hedonic eating. Plasma levels of anandamide (AEA), oleoylethanolamide (OEA) and palmitoylethanolamide (PEA), instead, progressively decreased in both eating conditions without significant differences.
AimsIn order to investigate the physiology of endocannabinoids in obesity, we assessed the responses of AEA, 2-AG, OEA and PEA to hedonic and non-hedonic eating in obese individuals.
MethodsFourteen satiated obese patients consumed favorite (hedonic eating) and non-favorite (non-hedonic eating) foods in two experimental sessions. During the tests, blood was collected to measure peripheral levels of AEA, 2-AG, OEA and PEA.
ResultsPlasma levels of 2-AG progressively decreased in non-hedonic eating whereas they gradually increased after hedonic eating. Plasma levels of AEA decreased progressively in non-hedonic eating, whereas they initially decreased after the exposure to the favorite food and then returned to baseline values after its consumption. The responses of OEA and PEA to favorite and non-favorite food did not show significant differences.
ConclusionsThese findings demonstrate that, compared to normal weight healthy subjects, obese subjects exhibit different responses of peripheral endocannabinoids to the ingestion of food for pleasure and this could have implications for the onset/maintenance of obesity.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Ghrelin response to hedonic eating in underweight and short-term weight restored patients with anorexia nervosa
- G. Fico, A.M. Monteleone, M. Nigro, G. Patriciello, U. Volpe, P. Monteleone
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S550
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Recently, anorexia nervosa (AN) has been conceptualized as a reward-related disorder, and brain imaging studies have shown functional and structural abnormalities in areas of the brain involved in reward processes in both acute and recovered AN patients. However, the role of endogenous biochemical mediators, such as Ghrelin, in the modulation of reward processes has been poorly investigated in this eating disorder.
ObjectivesHedonic eating, that is the consumption of food exclusively for pleasure and not to maintain energy homeostasis, is a useful paradigm to investigate the physiology of food-related reward.
AimsWe assessed the Ghrelin response to food-related reward in symptomatic AN women in order to further explore the modulation of reward processes in this severe and debilitating disorder.
MethodsPlasma levels of Ghrelin were measured in 7 underweight and 7 recently weight-restored satiated AN patients before and after the ingestion of a favorite (hedonic eating) and non-favorite (non-hedonic eating) food. Ghrelin responses were compared it that of previously studied healthy controls.
ResultsWe found that in satiated underweight patients with AN plasma Ghrelin levels progressively decreased after the exposure and the consumption of both the favorite and non-favorite food whereas in satiated weight-restored AN patients and satiated healthy controls plasma Ghrelin concentrations significantly increased after the exposure to the favorite food and after eating it, but decreased after the non-favorite food.
ConclusionsThese results suggest a derangement in the Ghrelin modulation of food-related pleasurable and rewarding feelings, which might sustain the reduced motivation toward food intake of acute AN patients.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Impaired cortisol awakening response in eating disorder women with childhood trauma exposure: evidence for a dose-dependent effect of the traumatic load
- A. M. Monteleone, P. Monteleone, U. Volpe, F. De Riso, G. Fico, R. Giugliano, M. Nigro, M. Maj
-
- Journal:
- Psychological Medicine / Volume 48 / Issue 6 / April 2018
- Published online by Cambridge University Press:
- 29 August 2017, pp. 952-960
-
- Article
- Export citation
-
Background
Childhood trauma is a non specific risk factor for adult eating disorders (ED), and the hypothalamic-pituitary-adrenal (HPA) axis seems to mediate such a risk. Here we explored the impact of different types of childhood trauma and of traumatic load on the cortisol awakening response (CAR) of women with anorexia nervosa (AN) or bulimia nervosa (BN).
MethodsSaliva samples were collected at awakening and after 15, 30, 60 min to measure cortisol levels by 121 women (44 AN patients, 36 BN patients and 41 healthy women). Participants filled in the Childhood Trauma Questionnaire.
ResultsAN and BN patients with childhood maltreatment exhibited an attenuated CAR compared with non-maltreated ones. In the whole ED patient group, the CAR showed a progressive impairment with the increasing number of reported trauma types. Although significant negative correlations emerged between the type or the number of traumas and the CAR, only the number of traumas remained significantly associated with the CAR in a stepwise multiple regression analysis.
ConclusionsPresent findings confirm that childhood trauma is associated with an impaired CAR in adult AN and BN patients and demonstrate for the first time a negative dose-dependent effect of the traumatic load on HPA axis activity.









